
For practice owners, patient scheduling is a core driver of revenue and operational efficiency. Your appointment system directly impacts patient throughput, staff workload, and overall profitability. Crucially, it is a key factor that determines your practice’s valuation during a sale.
This guide outlines how to optimize your scheduling models to improve daily performance now and maximize your enterprise value later.
What is Patient Scheduling Optimization?
Patient scheduling optimization is a data-driven method for organizing appointments to balance patient access, provider productivity, and resource use. Unlike traditional scheduling that simply fills time slots, optimization uses data to manage variables like no-shows, late arrivals, and appointment length variations. The goal is to increase patient throughput while maintaining high-quality care.
Inefficiencies are costly. A single no-show can cost over $100, and a practice with 20 no-shows per week can lose over $100,000 in annual revenue. When buyers perform financial due diligence, they scrutinize these operational metrics. An optimized schedule adds to your valuation; a chaotic one becomes a significant red flag.
Key Takeaway: A single no-show can cost over $100. For a practice with just 20 no-shows per week, that translates to over $100,000 in lost annual revenue.
How Does Scheduling Efficiency Impact Your Practice Valuation?
Buyers evaluate your practice based on the systems that generate revenue, not just the revenue itself. Efficient scheduling demonstrates operational maturity, which commands premium multiples.
An optimized schedule directly boosts your Adjusted EBITDA, the primary driver of most healthcare valuations. By seeing more patients without a proportional increase in overhead, you improve profitability and enterprise value. Buyers analyze patient throughput to identify growth capacity that does not require new capital investment.
Modern scheduling technology also signals scalability to buyers. Systems using AI and automation reduce dependency on specific staff members, demonstrating that the practice is built to scale. This is often achieved through a Management Services Organization (MSO) structure, which separates business operations from clinical care.
Strong operational metrics, such as high fill rates and low no-show rates, reduce perceived risk. Lower risk justifies higher valuation multiples. Ultimately, a practice with systems that function independent of the owner has demonstrable, transferable value. Buyers pay more when they are confident the practice will not collapse after you exit.
What Are the Most Common Scheduling Models?

Most successful practices use a hybrid approach, combining different models to fit various clinical and operational needs. Understanding the fundamental models is the first step to building a superior system.
| Scheduling Model | How It Works | Best For | Potential Pitfalls |
| Time-Slot | Each patient receives a specific, fixed appointment time (e.g., 9:00, 9:15). | Specialties with highly predictable appointment durations, such as surgical consults or procedures. | Delays cascade, creating long waits. No-shows create unproductive gaps in the provider’s day. |
| Wave Scheduling | Multiple patients (typically 2-4) are scheduled at the top of the hour and seen in the order they are ready. | Primary care and outpatient clinics with high volume and variability in visit length. | Can create an initial rush and longer waits for some patients if not managed by skilled staff. |
| Modified Wave | Patients are scheduled in the first half of the hour, leaving the second half open for catch-up, walk-ins, or urgent cases. | Practices needing same-day access, such as pediatrics or primary care during flu season. | Risks underutilizing provider time if the open slots are not consistently filled. |
| Double Booking | Two patients are intentionally scheduled in the same time slot. | Strategically managing high no-show patient populations or accommodating urgent add-ons. | Creates significant patient dissatisfaction and staff stress if both patients arrive on time. |
| Cluster Scheduling | Similar appointments (e.g., new patients, post-op checks) are grouped into specific time blocks. | Practices using specialized equipment or staff for certain visits; improves efficiency through repetition. | Can be inconvenient for patients and may lead to long wait times for a specific appointment type. |
| Open Booking | The schedule is kept largely open, with most appointments booked for the same or next day. | Urgent care clinics and primary care practices focused on maximizing patient access. | Difficult for patients who need to plan ahead and challenging to manage for specialty follow-ups. |
Which Scheduling Model is Best for My Practice?
There is no single “best” method. The optimal approach is a hybrid model tailored to your specialty, patient base, and operational goals. However, research points toward a few core principles.
Most outpatient practices benefit from using wave scheduling as a baseline. It naturally absorbs the unpredictability of daily operations—late arrivals, no-shows, and appointments that run long or short. A common variant is to schedule two established patients at the top of the hour and one new patient at the half-hour.
From there, sophisticated practices layer other strategies. They may use cluster scheduling for procedures and protect time slots for urgent visits using a modified wave. They abandon rigid 15-minute blocks in favor of data-informed time allocations based on actual visit lengths.
A specialized strategy is the 40/20 appointment model, which is effective when a patient requires multiple services in one visit (e.g., ophthalmology). One patient is scheduled at the top of the hour, and a second is scheduled at the 20-minute mark. This staggered flow maximizes resource use and minimizes patient wait times between services.
Pro Tip: The most effective “algorithm” for your practice is not a complex formula but a set of consistent, evidence-based principles. A systematic, data-informed approach using AI will always outperform scheduling based on intuition.
How Does Technology Improve Scheduling Performance?
Modern scheduling technology transforms practice operations and generates the clean data that buyers value. AI-powered platforms can predict appointment durations and identify high-risk no-show patients, with some practices reducing no-shows by up to 30%.
Patient self-scheduling is a critical feature, as 84% of patients prefer to book online. It frees up staff and fills schedule gaps, with over a quarter of online bookings often being for same-day or next-day appointments.
Automated, multi-channel reminders (text, email, phone) allow patients to confirm or reschedule with a single click, improving confirmation rates by 60% and reducing no-shows. When cancellations do occur, automated waitlist management instantly notifies other patients, turning a potential revenue loss into a filled appointment.
For owners planning an exit, this technology demonstrates operational maturity. It proves your practice’s efficiency is rooted in scalable systems, which helps avoid the common technology and EMR integration challenges that can complicate a sale and justifies a premium valuation.
What Scheduling Metrics Do Buyers Actually Scrutinize?
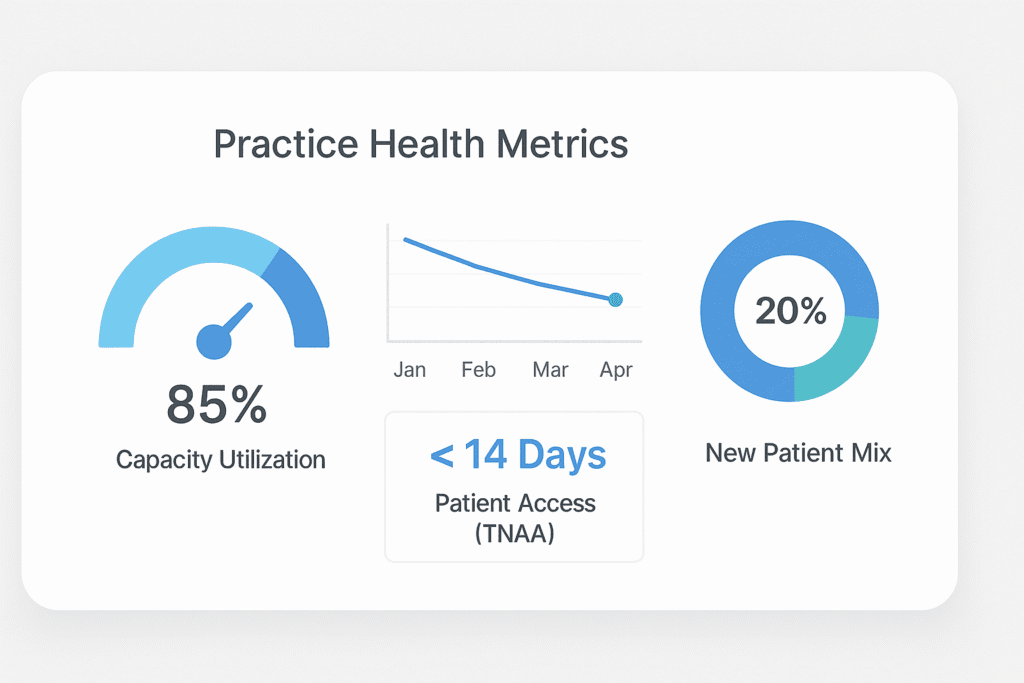
During due diligence, buyers analyze operational metrics to assess efficiency, growth potential, and risk. Your scheduling performance is central to this analysis.
- Patient Throughput and Capacity Utilization: Buyers calculate appointments per provider per day. A practice operating at 80-85% capacity is often more attractive than one at 95%, as it signals a clear runway for growth.
- No-Show and Cancellation Rates: Rates above the industry benchmark of 5-8% are a red flag. Buyers will also assess your response, as a strong patient engagement platform can mitigate this risk.
- Third-Next-Available Appointment (TNAA): This metric measures patient access. A TNAA of less than two weeks suggests strong, well-managed demand.
- New Patient Mix and Access: The ability to see new patients within two weeks, while maintaining a new patient mix of 15-20%, demonstrates a healthy, growing practice.
- Schedule Template Effectiveness: Buyers look for documented, standardized schedule templates. This indicates mature, predictable operations that can be easily transferred to new ownership.
- Data Quality and Technology Adoption: The ability to quickly produce reports on key scheduling metrics from your practice management system signals a level of operational sophistication that buyers reward with higher multiples, as it simplifies their analysis of your practice’s EBITDA.
Valuation Insight: Buyers often find practices operating at 80-85% capacity more attractive than those at 95%. This signals a clear runway for growth without requiring new capital investment.
How Can I Optimize My Current Scheduling System?
You can achieve significant gains without a complete overhaul. Following a practical roadmap for systematic improvement is a key component of effective healthcare practice management.
First, gather baseline data. Track actual appointment durations by type, calculate no-show rates, and identify your peak and slow periods for at least four weeks. This data will reveal your biggest opportunities.
Next, transition to a modified wave schedule for routine appointments. Start with one provider to pilot the change. Use your data to assign realistic time allocations for different visit types instead of treating all appointments as identical.
Then, build in strategic buffer time—30-60 minutes of unbooked time, typically mid-morning and mid-afternoon. This planned flexibility absorbs delays and creates capacity for urgent additions.
Implement automated reminders and an active waitlist. These two technological interventions can dramatically reduce no-shows and ensure cancellations are filled immediately. Finally, train your front office staff on the why behind your scheduling strategy. Empowered staff make better real-time decisions that align with your operational goals.
When Should I Optimize Scheduling Before Selling Your Practice?
If you plan to sell within the next 2-5 years, the time to optimize your scheduling is now.
Buyers pay for proven performance, not potential. By optimizing 18-36 months before a transaction, you create a documented track record of improving patient throughput, declining no-show rates, and increasing EBITDA. This sustained performance history, often validated through a Quality of Earnings (QoE) analysis, reduces buyer risk and is a key strategy to maximize the valuation of your healthcare practice.
This lead time also allows you to work through implementation challenges without the pressure of a pending transaction. You can test different approaches, train staff properly, and refine your system to find what works best for your specific practice.
The Strategic Value of Scheduling Optimization
Patient scheduling is a strategic asset. For practice owners focused on current performance, optimization leads directly to higher patient volume, lower staff stress, and greater profitability.
For those positioning for a future sale, it is one of the most direct ways to enhance enterprise value. An optimized scheduling system demonstrates operational maturity, generates the clean data buyers demand, and directly boosts the EBITDA that underpins your valuation.
The time to start is now. By treating your schedule as a core component of your business strategy, you will build a more efficient, more profitable, and ultimately, more valuable practice.
Build a More Valuable Practice
Optimizing your scheduling is a critical first step, but it is one part of a larger strategy to maximize your practice’s enterprise value. Our team at SovDoc specializes in helping practice owners prepare for and navigate successful transactions.



